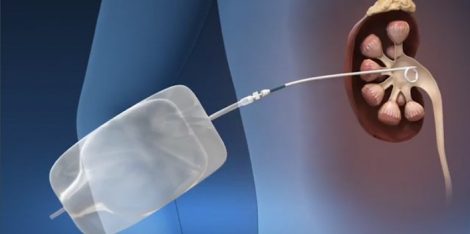
Percutaneous nephrolithotomy (PCNL) is a procedure used to remove kidney stones from the body when they are too large and cannot pass on their own. This procedure uses small telescopes (also called nephroscopes) and instruments inserted through a small incision in your back to break up/fragment the kidney stones and remove their fragments. Percutaneous nephrolithotomy is used most often for larger stones or when other procedures, such as extracorporeal shock wave lithotripsy or ureteroscopy, are unsuccessful or not possible.
Therefore, PCNL is used for larger, stones that are harder in chemical composition, or are unsuccessful with other treatment options.
What are the advantages?
- Allows large or complicated stones to be treated in a minimally invasive fashion, where in the past this would have necessitated a large skin incision.
- Hospital stay is usually overnight, and out of hospital recovery time is significantly shorter than traditional open surgery.
What are the disadvantages?
- Compared to traditional treatments of large complex stones, there are no disadvantages. Improved techniques and equipment have allowed this type of surgery to be safer than ever before.
- This procedure is usually preformed at specialized centers with specialized equipment and appropriate medical personnel.
What Preparation is Required?
You will be required to have detailed imaging, such as CT scans, to allow the surgeon to assess the stone in fine detail regarding its relationship to the kidney and nearby structures. This will enable the surgeon to plan the best access point(s) to the kidney to allow effective clearance of stones.
As the procedure is performed under general anaesthesia, you should have nothing to eat or drink for 6 hours prior to treatment. Regular medications can be taken with a sip of water with the exception of blood thinning agents (eg. warfarin, aspirin, clopidogrel) or non-steroidal anti-inflammatories which need to be stopped for 7-10 days. A mid stream urine (MSU) test is required to ensure the urine is sterile before treatment is undertaken. Other tests required include urine culture, kidney function studies, and complete blood counts. These tests will all be organized from the rooms after your consultation.
What are the risks?
This form of surgery is low risk if performed by an urologist who is specifically trained in this technique, and aided by meticulous pre-operative planning. The specific risks are uncommon but include infection, excessive bleeding (necessitating blood transfusion 2%, embolisation 1%, renal exploration 0.5%), and adjacent organ injury (spleen, liver, bowel, and lung).
What do I need to bring to surgery?
- All related available imaging such as KUB (kidneys, ureter, and bladder) x-ray, CT scan abdomen, or kidney ultrasound. All of these x-rays and images can be brought on a cd/disc.
- Your usual medications
What happens in the operating room?
The procedure is done in three steps. First, a cystoscopy is performed, where the surgeon will image your kidney stone to make sure there is no blockage. Second, you will be taken to thew Interventional Radiology suite for precise placement of an access tube into the kidney. Finally, this access is used by your urologist to fragment and remove your kidney stones. It is a team effort requiring coordination from the surgeons and nursing staff.
What to expect afterwards?
You will have a temporary catheter called a nephrostomy tube draining the kidney, as well as a urinary catheter, draining your bladder. They will be removed prior to discharge from hospital. The urine will be bloodstained for up to a week after discharge from hospital. Imaging is performed immediately after surgery to assess stone clearance. Occasionally, further minor surgery may be required to clear any remaining stones to achieve complete stone clearance. Your hospital stay will be 1-2 days on average.
Follow Up
You will be required to take it easy during the recovery phase for several weeks. If you don’t follow these instructions, you may have bleeding from the kidney — a serious problem. There should only be minimal discomfort from the wound. Oral antibiotics will be given for a further five days to prevent infection. It is important to inform us if you feel unwell with fevers, chills, or develop heavy bleeding in the urine. Your initial follow-up will be in 6 weeks after discharge. Usually, a urinary stent is left to ensure the urine drains correctly into the bladder. This will require removal at a later time.